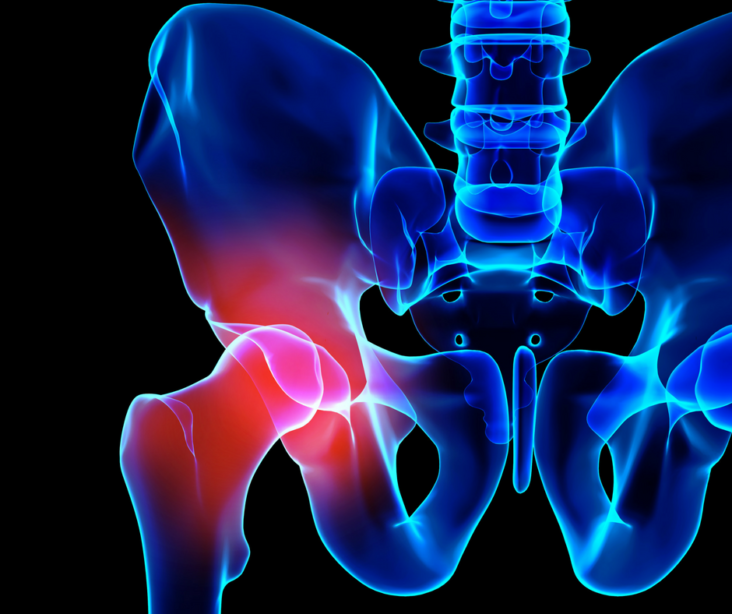
Stenosis is a common spinal condition caused by arthritic build up in the joints (facet joints) and ligaments in the lower back. In addition, one may have a disc bulging that causes pressure on the nerves passing through the narrow canal.
Symptoms:
Back and leg pain down one or both legs, numbness or tingling, weakness often associated with electric shocks running from the back to the feet. These symptoms are increasingly aggravated, at a varying degree while walking, and improve when sitting or stooping forward.