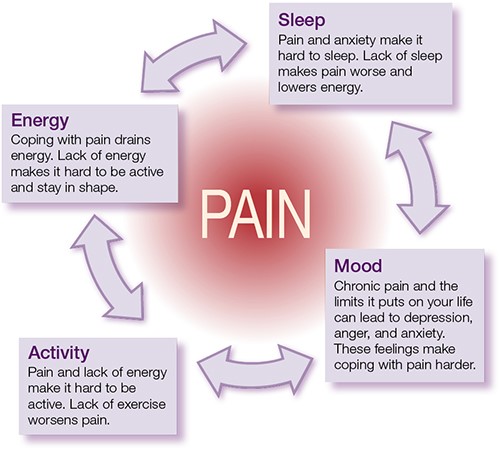
Are you struggling with sciatic nerve pain or spinal instability that’s interfering with your daily life? Traditional spinal surgeries often require long recovery times and can be quite invasive. However, thanks to the revolutionary S-LIF (Supine Lateral Interbody Fusion) technology, there’s now a far less invasive option for lumbar fusion surgery.
Developed exclusively at Legacy Spine & Neurological Specialists, the S-LIF is transforming spinal surgery by offering patients a minimally invasive approach with faster recovery times and fewer complications.
What is the S-LIF Procedure?
The S-LIF is currently the least invasive option for lumbar fusion surgery available worldwide. This advanced procedure is a step beyond the MIG-LIF procedure, which was first developed by Dr. Scott Schlesinger in 2015. MIG-LIF was a groundbreaking outpatient surgery performed through a keyhole incision, but Dr. Schlesinger saw room for further improvement.
By applying his expertise in microsurgical techniques—honed through years of performing complex brain surgeries—Dr. Schlesinger developed the S-LIF, making it even less invasive than its predecessor. Today, S-LIF offers a state-of-the-art solution for patients requiring decompression and fusion of the lumbar spine, using the smallest possible incision.
Who is a Candidate for S-LIF?
While the S-LIF procedure is an exceptional option for many, it is not suitable for all patients. Some individuals with more severe spine conditions may still require traditional, more invasive surgery. However, for patients who qualify, the benefits are substantial. If you’re suffering from sciatic pain, compressed nerves, or spinal instability, this could be the ideal minimally invasive solution to restore your quality of life.
Why Choose S-LIF?
Here’s why S-LIF stands out among lumbar fusion surgeries:
- Minimally Invasive: Performed through a keyhole incision, leading to less pain and faster recovery times.
- Outpatient Procedure: No need for an extended hospital stay. You can return home the same day.
- Faster Recovery: Patients experience significantly shorter recovery periods compared to traditional lumbar fusion surgeries.
- Reduced Risk: Lower complication rates due to its less invasive nature.
Meet the Pioneers of S-LIF at Legacy Spine & Neurological Specialists
The S-LIF procedure is exclusively performed by Scott Schlesinger, MD, and Dominic Maggio, MD, two of the top neurosurgeons in the country.
Dr. Scott Schlesinger, MD
Dr. Schlesinger has been a leading neurosurgeon since 1992. He trained at UT Southwestern and completed a fellowship in Lausanne, Switzerland. Over his career, Dr. Schlesinger has been recognized with numerous awards and accolades, consistently being named among the Best Neurosurgeons in the state. As the founder of Legacy Spine and Neurological Specialists, Dr. Schlesinger developed the S-LIF procedure, using his microsurgical expertise to push the boundaries of minimally invasive spine surgery.
Dr. Dominic Maggio, MD
Dr. Maggio joined the Legacy Spine team in July 2021 and has quickly established himself as an outstanding surgeon specializing in both the S-LIF procedure and other advanced spinal surgeries. Dr. Maggio trained at the University of Virginia-National Institutes of Health neurosurgery program and completed a fellowship at Ohio State University. His skill set includes complex and minimally invasive spine surgery techniques, for which he has received multiple awards for both his research and clinical expertise.
Is S-LIF Right for You?
If you’re tired of living with back pain or numbness caused by spinal issues, the S-LIF procedure could be the life-changing solution you need. Not all patients are candidates, but for those who are, this procedure offers the least invasive option for lumbar fusion surgery available today.
Contact Legacy Spine & Neurological Specialists Today
Want to learn more about S-LIF or find out if you’re a candidate for this cutting-edge procedure? Call us today or send us a message through our website. Our dedicated team is ready to help you on the path to a pain-free life.