All too often a patient will come into clinic that has been very diligent with a fitness regime for years but despite preemptive health measures the patient will develop low back pain. It is described as a deep ache that is worse in the morning and/or night begins to interfere with the normal activities of his/her day. Seems like such a waste of time to put all the effort into staying fit then still having pain, right?
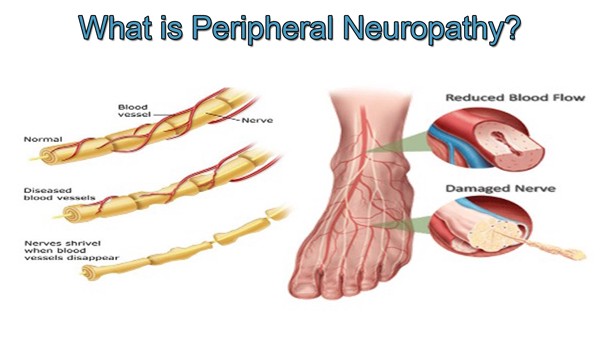
Often there is no specific injury and very little diagnostic grounds other than “facet hypertrophy” (described normally as arthritis in the low back) to support the claim of this pain. Chances are with most of these patients, arthritis did not develop in the last week or month. It is an accumulation of years of repetitive weightbearing and compressive forces to the spine that have brought about this change. The question remains, what can be done to improve this pain when you already believed you were doing all the right things to stay healthy?
In terms of treatment with patients that present with the history that I have outlined above; moderation becomes a recurrent phrase of emphasis. Other useful tools are variation and observation. Mixing up the cardio routine with a variation of biking (indoor or outdoor), swimming, and walking. If you have a gym routine for lifting weights or resistance exercises, try mixing things up by doing body weight activities or group aerobics. It may also be a nice change of pace to do a beginner’s class of yoga or Pilates. Moderation and observation are key parts to avoiding overuse injuries that cause setbacks.
There is current research to suggest that indeed there is a “happy medium” to activity. Too much activity can have as much of a negative impact on the body as doing nothing at all. Take home points:
- Use Variation in exercise choice
- Practice moderation with strenuous activities
- Observe how your body responds to activity and modify if necessary
If you are having setbacks due to low back/neck pain from too much activity or you find yourself sedentary and have no idea where to start, give us a call at 501-661-0077 for a consultation and evaluation at Legacy Spine and Neurological Specialists so that we can get you Back to Life!